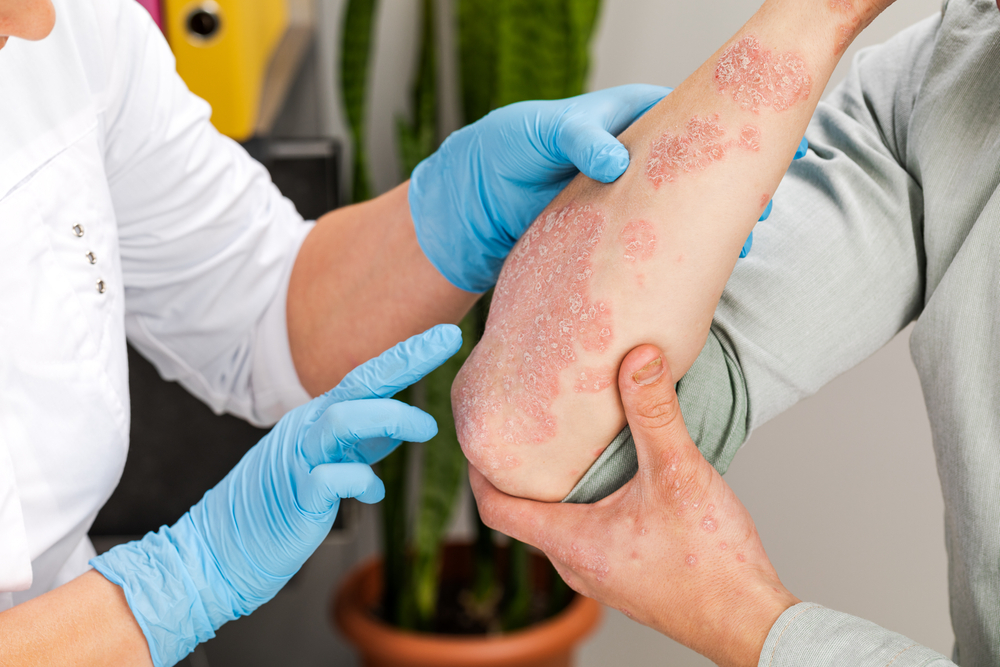
In order to determine the association between rhegmatogenous retinal detachment (RD) and atopic dermatitis (AD), researchers retrospectively reviewed medical records of patients who underwent RD surgery at a single clinic. In patients with AD, they found that RD occurred at a young age with different characteristics and a poor prognosis for visual acuity when compared to non-AD patients. The results of the study were published in BMC Ophthalmology.
Given the additional risks associated with RD in patients with AD, “extensive treatment and management are needed for these patients,” according to the study’s lead author, Youlim Lee. “Moreover, atopic patients had a much higher risk of RD after cataract surgery than controls. Thus, careful examination should be performed regularly for atopic patients after a cataract surgery to achieve the best patient outcomes,” Lee added.
Among the 2,257 reviewed medical records of patients who underwent RD surgery, 61 patients diagnosed with AD were identified and assigned into the experimental group. Records from 100 patients who did not have AD were randomly selected and assigned to a control group. The primary datapoints assessed were demographics, characteristics of detachment, initial operative method, and prognosis after surgery. Researchers also measured the time between cataract surgery and onset of RD in pseudophakic RD patients.
The researchers observed that postoperative visual acuity and prognosis were significantly worse, and bilateral involvement of RD was more common in the atopy group than in the control group (p = 0.005, 0.001). RD presented with different characteristics in the two groups.
Of note, researchers found that the risk of RD within one year after cataract surgery was significantly higher in pseudophakic patients of the atopic group than in the control group (p = 0.013). There was no significant difference in mean preoperative visual acuity, or refractive index between the two groups.
The authors acknowledged some limitations of the study, such as its retrospective design, small sample size, and relatively short follow up period. However, they asserted that their results showed that RD occurs at a younger age with different characteristics in patients with AD versus non-AD patients, and careful management is necessary. The author’s report closed by calling for further studies with a longer follow-up and a larger sample to deepen understanding of the association between AD and RD.
Source: BMC Ophthalmology