Watch this engaging conversation between study author Valentina Puntmann, MD, and DocWire News Cardiology Section Adviser Payal Kohli, MD, about the fallout from Dre. Puntmann’s important JAMA Cardiology paper reporting cardiovascular outcomes assessed by MRI in patients who had COVID-19. The study was one of the factors that caused some institutions (like those in the Big 10) to put their fall sports seasons on hold.
VIDEO: Cardiovascular MRI Outcomes in Patients Recovered from COVID-19 (Part 1)
–
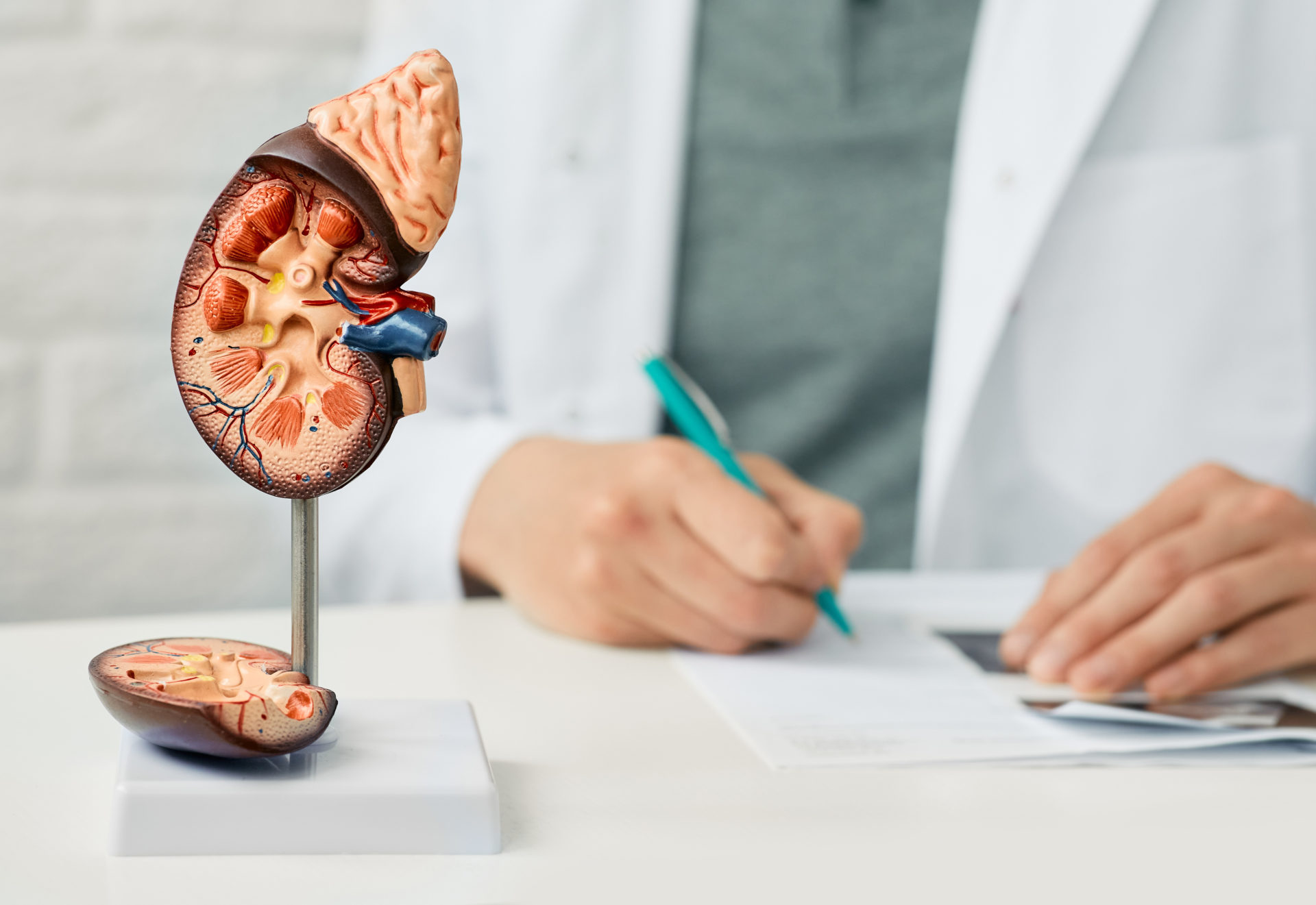
In this study, atrial septal defect (ASD) closure patients with no history of migraines were randomized 1:1 to receive aspirin plus clopidogrel (n=84) or aspirin plus placebo (n=87) for three months after the procedure; after the first three months, only aspirin was used. Patients were followed up at three, six, and 12 months via a migraine headache questionnaire. The primary outcome was incidence and severity of migraine attacks at six and 12 months. “Adding clopidogrel to aspirin for 3 months after transcatheter atrial septal defect (ASD) closure results in a lower incidence of new-onset migraine attacks. However, the outcomes at 6- to 12-month follow-up (after clopidogrel cessation at 3 months) remain largely unknown,” the researchers wrote in their reasoning for undertaking the study.
–
Researchers for this study conducted a community-based participatory project in conjunction with a community health organization, a primary care center, and a digital health company. The overwhelming majority of participants were interested in engaging with the study. A total of 81 ELP and 50 SLP were enrolled in the study. The researchers noted that participants liked having access to their health records and were comfortable sharing data on health devices suck as FitBits and blood pressure cuffs. Compared with pre-study, the participants were much more comfortable using mHealth apps and to participate in research that used apps. Participants were also interested in further functionality of the apps, and for using them to bring knowledge or information about the conditions to others they may know with the condition.
mHealth Initiative Well-received by Study Population, Researchers Report
–
While Still High, Recurrent Heart Attacks are on the Decline
This study included data from more than 770,000 U.S. women and 700,000 U.S. men < 65 years of age who had a myocardial infarction (MI) hospitalization between 2008 and 2017. Patients were followed the participants for recurrent MI, current coronary heart disease events (such as recurrent MI or coronary revascularization), heart failure hospitalization, and all-cause mortality for one year post-initial MI. The age-standardized rate of recurrent MI per 1,000 person-years decreased from 89.2 to 72.3 in women and from 94.2 to 81.3 in men (P for interaction by sex<0.001). They also reported that recurrent rates of coronary heart disease events also decreased from 166.3 to 133.3 in women and from 198.1 to 176.8 in men (P for interaction<0.001).
–
Credit: Original article published here.