A new study found that certain treatments for non-hematological cancers may be associated with changes and disruptions to patient gut health.
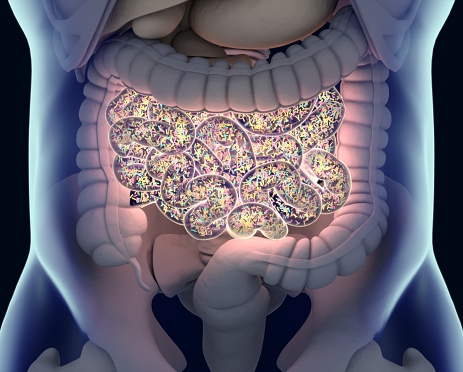
This study, published in BMC Cancer, evaluated the impact of myelosuppressive chemotherapy on gut microbiota in humans with solid tumors and non-hematologic malignancy.
“We know that myelosuppressive chemotherapy reduces white blood cell count significantly during the first seven to 10 days of treatment, making the body more vulnerable to infection,” lead author Lito Papanicolas, infectious diseases expert and PhD candidate at the South Australian Health and Medical Research Institute (SAHMRI) and Flinders University, said via press release. “In this study we focused on how much the individual’s microbiome changed over this period, when the bacteria are most likely to cause infection.”
Gut Microbiome After Chemotherapy
The research team from SAHMRI assessed 19 patients with non-hematological malignancies who were being treated with chemotherapy but not antibiotics. Fecal samples were collected prior to treatment initiation, seven to 12 days after chemotherapy, and at the end of the first treatment cycle. The primary endpoint was gut microbiota diversity via 16S rRNA gene amplicon sequencing.
Patients’ gut microbiome changes significant pre- and post-chemotherapy, according to the authors. Samples collected seven to 12 days after initiation of chemotherapy showed increased richness and diversity of microbiota, with significantly reduced abundance of gram-positive bacteria and an increase in gram-negative bacteria. There was a relative increase in the presence of Proteobacteria, which the authors noted has previously been linked increased infection risk in patients with cancer. However, these differences did not remain significant by the end of the treatment cycle.
“In the absence of a driver of microbiome disruption, such as exposure to antibiotics, the composition of an individual’s gut microbiome typically remains relatively stable over time. However, paired analysis of microbiome composition before and after chemotherapy showed that microbiome composition variability was greater than expected, as there was far less temporal change occurring in healthy participants who did not receive chemotherapy over the same time interval,” wrote the study authors. “This suggests that chemotherapy, rather than natural temporal variability of samples, drives the changes to microbiome composition.”
The researchers note that further research is needed to determine whether alterations of the microbiome is actually necessary for treatment efficacy. “It could be that what we’re seeing is actually a good thing, because there’s a possibility that the change in microbiome triggers the body’s immune response to fighting cancer,” said Dr. Papanicolas.
Chemotherapy destabilizes the gut microbiome in cancer patients
Read: https://t.co/FGAHlbv5OU#USSLLC #health #Chemotherapy #cancerpatients pic.twitter.com/UKPjIrEEzU— Universal Stream Solution (@ussllc_) July 7, 2021
Myelosuppressive chemotherapy destabilises gut microbiome in patients with solid organ cancershttps://t.co/WHjtoqDRg9
— Massimo Barberi (@masbarberi) July 7, 2021
Credit: Original article published here.